Most people treat brushing and flossing like a cosmetic routine. Fresh breath. Whiter teeth. Fewer cavities. I used to think the same way until I started digging into how oral bacteria affect overall health and realized the mouth isn’t just a separate system. It’s a gateway.
The reality is uncomfortable. Your mouth holds more than 700 species of bacteria. Some protect you. Others quietly contribute to inflammation, vascular damage, metabolic issues, and even cognitive decline when they overgrow. Once that balance shifts, the effects don’t stay in your gums. They move.
The Oral Microbiome: More Than Just Plaque
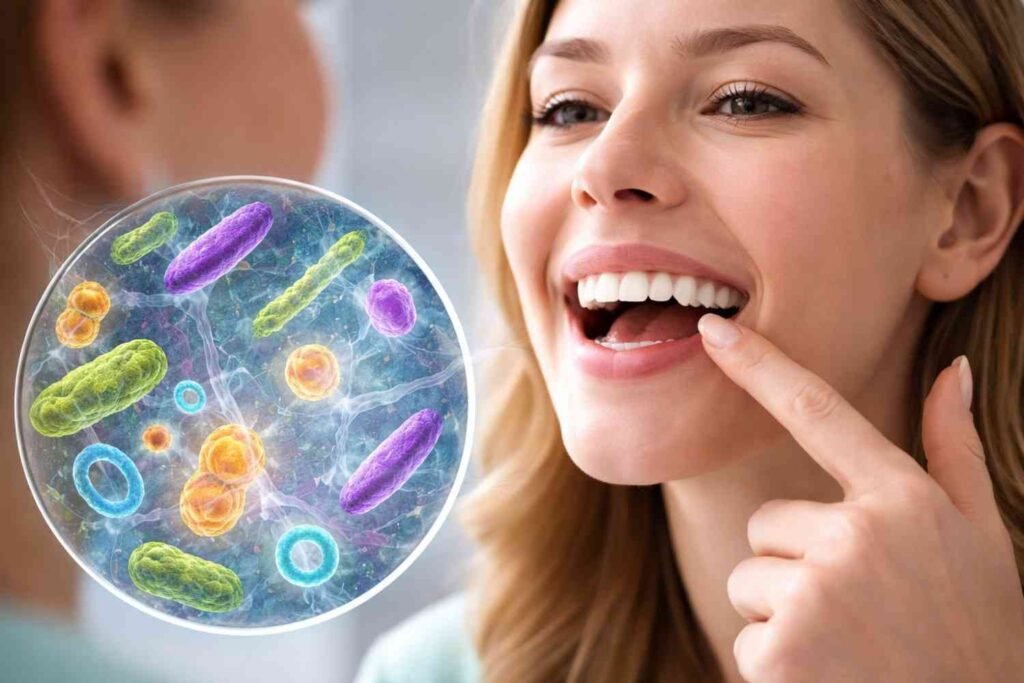
The oral microbiome is a living ecosystem. Under healthy conditions, it maintains balance. Saliva, immune defenses, and beneficial microbes keep harmful bacteria in check. But poor oral hygiene, high sugar intake, tobacco use, or unmanaged health conditions can disrupt this equilibrium.
When an imbalance occurs, known as oral microbial dysbiosis, harmful bacteria such as Porphyromonas gingivalis multiply. Inflamed gums become porous. Tiny blood vessels underneath irritated tissue allow bacteria and inflammatory molecules to enter circulation. That’s where the real story begins.
Systemic inflammation doesn’t feel dramatic at first. It’s low-grade, chronic, and often silent. But over time, it contributes to vascular damage, immune dysregulation, and metabolic instability. That’s the bridge connecting oral bacteria to chronic disease.
Cardiovascular Health: The Artery Connection
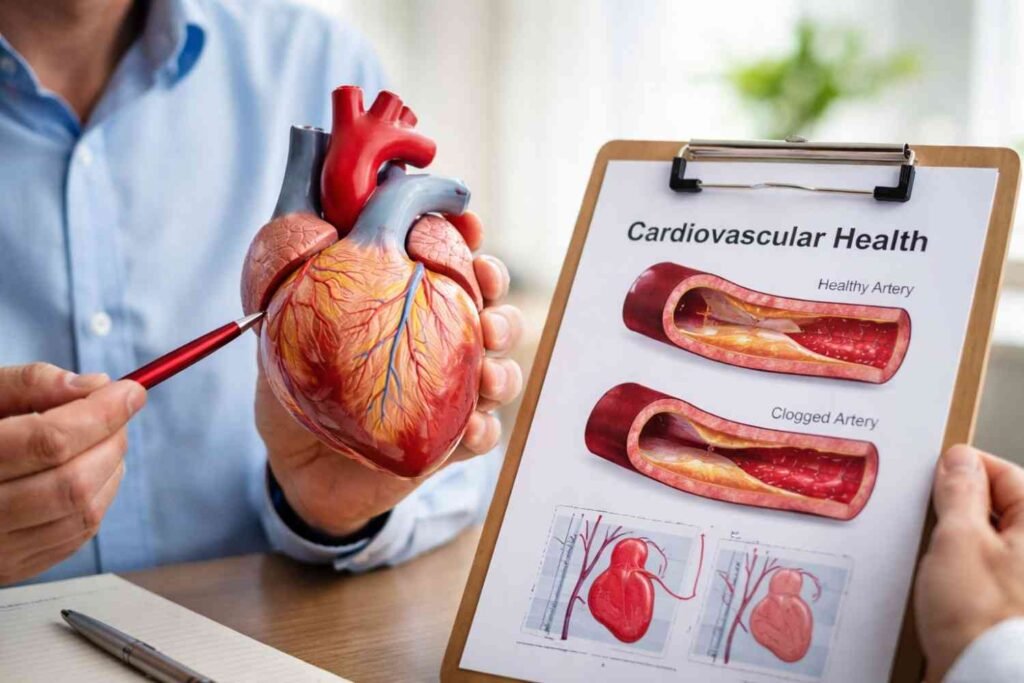
Researchers have detected periodontal pathogens inside arterial plaque. That finding changed how cardiologists think about gum disease. When bacteria enter the bloodstream (bacteremia), they can adhere to damaged arterial walls and accelerate plaque formation.
Adults with severe periodontal disease show significantly higher rates of heart attack and stroke. Inflammatory markers like IL-6 and TNF-alpha, released from infected gum tissue, circulate through the body and contribute to endothelial damage the earliest step in atherosclerosis.
This isn’t about occasional bleeding gums. It’s about persistent inflammation feeding vascular risk over the years.
Diabetes and Insulin Resistance: A Two-Way Street

The link between metabolic health and oral bacteria is bidirectional. Chronic gum infections increase systemic inflammation, which worsens insulin resistance. At the same time, elevated blood sugar creates an environment where harmful bacteria thrive.
People struggling with blood sugar control often experience more severe periodontal disease. And once gum disease progresses, it makes glucose regulation harder. It becomes a loop.
Addressing oral health doesn’t replace medical diabetes management, but improving gum health can reduce inflammatory load and support better metabolic stability.
Respiratory and Lung Complications
Oral bacteria don’t just enter the bloodstream. They can also be aspirated into the respiratory tract. Microscopic droplets of saliva carrying bacteria reach the lungs, especially during sleep or in individuals with compromised immunity.
This increases risk for:
- Pneumonia
- Chronic bronchitis
- Exacerbations of COPD and emphysema
For older adults or people with weakened immune systems, this pathway becomes especially significant.
Cognitive Decline and Brain Health

One of the more unsettling discoveries involves neurodegeneration. Researchers have detected oral bacteria in the brain tissue of individuals with Alzheimer’s disease. While causation is still under investigation, chronic inflammation appears to play a major role.
Inflammatory cytokines triggered by periodontal disease may cross the blood-brain barrier. Over time, this inflammatory burden could contribute to neuronal damage and memory decline. The oral-brain connection is no longer considered fringe science; it’s actively studied.
Digestive and Gut Microbiome Disruption
We often talk about the gut microbiome. What we don’t talk about enough is how the mouth feeds into it.
Harmful oral bacteria swallowed daily can alter gut microbial balance. Emerging research suggests this oral-gut axis may influence conditions like IBS, increased intestinal permeability, and chronic digestive inflammation.
The digestive tract doesn’t operate in isolation. It starts at the mouth.
Pregnancy and Systemic Impact
Severe periodontal disease has been associated with premature birth and low birth weight. Bacteria entering circulation can reach placental tissue and trigger inflammatory responses that affect fetal development.
For expectant mothers, gum health isn’t cosmetic. It’s preventive medicine.
How Oral Bacteria Affect Overall Health: The Three Main Pathways
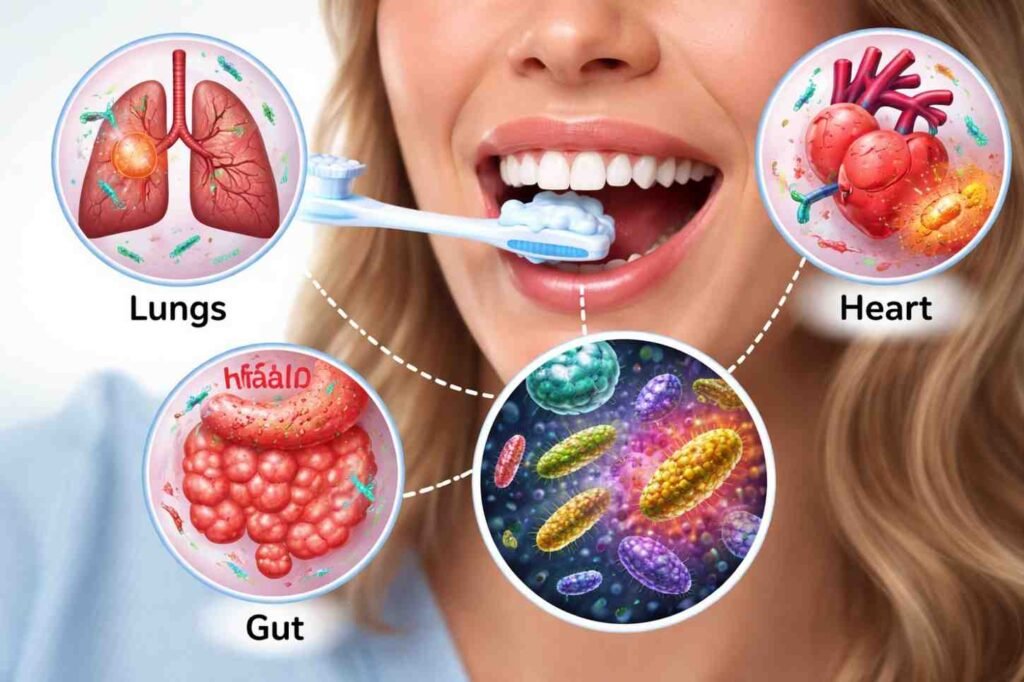
Research consistently highlights three mechanisms that explain how oral bacteria affect overall health:
- Bloodstream invasion (bacteremia): Bacteria enter circulation through inflamed gum tissue and travel to distant organs.
- Systemic inflammatory response: Cytokines released from infected gums circulate and damage vascular tissue.
- Aspiration into lungs: Bacteria are inhaled into the respiratory tract, increasing infection risk.
These pathways explain why oral health influences far more than teeth.
Practical Steps to Reduce Systemic Risk
Prevention doesn’t require extreme measures. It requires consistency.
- Visit a dentist twice yearly for professional cleanings.
- Brush twice daily with fluoride toothpaste.
- Floss daily to remove plaque between teeth.
- Limit refined sugar intake.
- Avoid tobacco, which impairs gum immunity.
Small habits reduce bacterial load and systemic inflammation over time.
Why This Matters More Than People Realize

Chronic diseases don’t develop overnight. They accumulate through years of subtle inflammation, immune stress, and metabolic strain. The mouth can quietly contribute to that burden.
When people ask how oral bacteria affect overall health, the answer isn’t dramatic, it’s cumulative. Every episode of untreated gum inflammation adds to systemic stress. Every year of neglected periodontal disease increases long-term risk.
The good news? Oral health remains one of the most controllable variables in preventive care. You can’t control genetics. But you can control your toothbrush.
Frequently Asked Questions (FAQs)
1. Can oral bacteria really enter the bloodstream?
Yes. Inflamed or bleeding gums create microscopic openings that allow bacteria to enter circulation. This process is called bacteremia and has been documented in periodontal disease.
2. Does improving gum health lower inflammation?
Research suggests that treating periodontal disease can reduce systemic inflammatory markers, which may support cardiovascular and metabolic health.
3. Is there a connection between oral bacteria and Alzheimer’s?
Oral pathogens have been detected in the brain tissue of Alzheimer’s patients. While research is ongoing, chronic inflammation appears to play a role in neurodegeneration.
4. How often should someone get professional dental cleanings?
Most dental professionals recommend cleanings twice per year, though individuals with gum disease may need more frequent visits.
Final Thoughts
For years, oral health was framed as cosmetic maintenance. That perspective no longer holds up. The mouth functions as an extension of the immune system, vascular system, respiratory system, and digestive system. When oral microbial balance breaks down, the ripple effects move far beyond cavities. Chronic inflammation, vascular damage, metabolic instability, and immune disruption often begin at surfaces people ignore.
Taking oral health seriously isn’t about vanity. It’s about reducing long-term systemic risk. And that shift in mindset changes everything.




